What Is the Pelvic Floor and Why It Matters for Everyone
Whether you’ve experienced pelvic pain, incontinence, or back issues—or you’re simply curious about how your body works—understanding the pelvic floor is essential. In this episode of The Code podcast, Dr. Andrew Fix talks with Dr. Katie Sasser to break down everything you need to know about pelvic floor health—for both women and men.
Meet Dr. Katie Sasser
Dr. Katie Sasser is a Doctor of Physical Therapy and pelvic floor specialist with over a decade of experience. After starting her career in orthopedics, she shifted her focus in 2021 after advanced pelvic health training. She now treats both orthopedic and pelvic conditions, helping patients reconnect with their bodies during life phases like pregnancy, postpartum, and menopause.
What Is the Pelvic Floor?
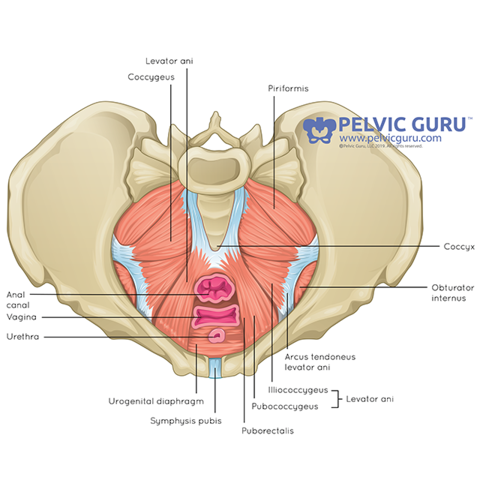
The pelvic floor is a bowl-shaped group of muscles at the base of the pelvis. These muscles:
-
Support internal organs
-
Stabilize the spine and hips
-
Control bladder and bowel function
-
Promote sexual function
-
Aid in fluid movement throughout the body
🧠 Dr. Sasser’s “A-Frame” Analogy:
-
Main floor → Resting tone
-
Attic → Contraction phase (sneeze, jump)
-
Basement → Relaxation phase (bowel movement)
Common Reasons to See a Pelvic Floor Therapist
For Women:
-
Pelvic, hip, or tailbone pain
-
Urinary or fecal incontinence
-
Pain with intercourse
-
Postpartum recovery
-
Prolapse symptoms
For Men:
-
Erectile dysfunction
-
Pelvic or testicular pain
-
Post-prostate surgery recovery
-
Incontinence or urgency
-
Pain with intimacy
💡 Yes—men have pelvic floors too!
Core, Stability, and the Pelvic Floor: It’s All Connected
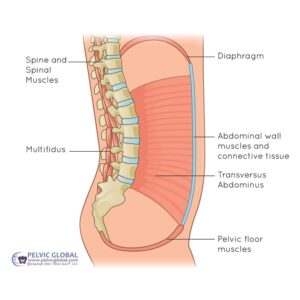
Your core is more than abs—it’s a pressure system:
-
Top: Diaphragm
-
Bottom: Pelvic floor
-
Front: Transverse & rectus abdominis
-
Sides: Obliques
-
Back: Erector spinae
A well-functioning core supports healthy movement, reduces back pain, and prevents incontinence. Proper bracing and breathwork are key—but rarely taught.
What to Expect During a Pelvic Floor Evaluation
-
History & Intake – Discuss “The 3 P’s”: Pee, Poop, and Pleasure
-
Internal Exam (with consent) – Gentle, one-finger vaginal assessment
-
Movement Screening – Observe pelvic floor response during activity
-
Compassionate Care – Your comfort and consent come first
Note: Internal work is never required for treatment.
External Pelvic Floor Therapy Options
If internal work isn’t for you, treatment may include:
-
Breathwork and pressure control
-
Functional movement coaching
-
Glute and hip strengthening
-
Postural and core engagement training
Stress, Breath, and Pelvic Health
Chronic tension—especially in the jaw, core, or pelvis—can overload the pelvic floor. Katie often starts treatment with breathwork and mindful relaxation to help the pelvic floor “reset.”

Quick Tips for Better Pelvic Floor Health
-
⏱ Urination should last ~14 seconds
-
📵 Avoid scrolling on the toilet
-
🛁 Relax your pelvic floor daily—not everything is about tightening
-
😮💨 Sync breath with pelvic floor movement
-
🧠 Manage stress through breathwork, therapy, or lifestyle changes
Closing the Gap in Women’s Health
Dr. Sasser advocates for:
-
Postpartum moms – Care beyond the 6-week checkup
-
Perimenopausal & menopausal women – Addressing hormonal impact on pelvic health
“Being a mom is hard. Going through menopause is hard. But being weak in those phases is even harder.” – Dr. Katie Sasser
Not in Colorado? We Can Still Help.
Virtual consultations are available for guidance and local referrals.
📧 Email: katie@physioroomco.com
📱 Instagram: @dr.katiesasser.dpt
Ready to Take the First Step?
If something here resonated with you, pelvic floor therapy could be transformative. Our team at Physio Room is here to help.
👉 Book an Appointment | Learn More About Our Services
🎧 Listen to the full podcast episode: Pelvic Floor Physical Therapy Explained with Dr. Katie Sasser

Written by Dr. Katie Sasser – PT, DPT, M.Ed.| Physio Room



Connect with Physio Room:
Find Us On Our Socials
Website
Instagram
Facebook